What are GLP-1 RA drugs?
 Glucagon-like peptide-1 receptor agonists (GLP-1 RA) have emerged as revolutionary drugs for chronic weight management. They are rapidly gaining popularity due to their effectiveness in helping patients lose weight. Examples of once-weekly injectable GLP-1 RA drugs include Ozempic (semaglutide), Trulicity (dulaglutide), and Mounjaro (tirzepatide).
Glucagon-like peptide-1 receptor agonists (GLP-1 RA) have emerged as revolutionary drugs for chronic weight management. They are rapidly gaining popularity due to their effectiveness in helping patients lose weight. Examples of once-weekly injectable GLP-1 RA drugs include Ozempic (semaglutide), Trulicity (dulaglutide), and Mounjaro (tirzepatide).
Safety risk under anesthesia
However, there are concerns regarding the safety of patients taking GLP-1 RA when undergoing anesthesia for elective procedures. The primary concern is the increased risk of aspiration, which occurs when the gastric contents rise up the esophagus (food pipe) and enter the trachea (windpipe). If this happens during airway management, it can cause damage to the lungs.
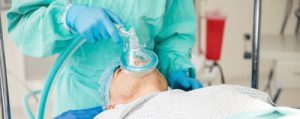
To minimize their risk of aspiration under anesthesia, patients are required to fast for several hours before their procedure to allow the stomach to “empty.” This is where GLP-1 RAs can cause problems. Since these drugs induce gastroparesis (slowing down of the stomach’s emptying), a patient on a GLP-1 RA can have a “full” stomach even after fasting for the generally recommended times.
Our research study on GLP-1 RA risks with anesthesia
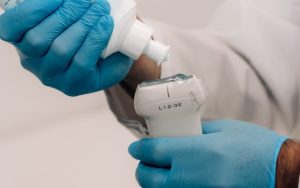 One way to figure out if the stomach is “full” (unsafe) or “empty” (safe) before anesthesia is using ultrasound to look at the stomach contents. Point-of-care ultrasound (POCUS) is a validated and accurate technique that can be useful but requires additional training and expertise from anesthesiologists.
One way to figure out if the stomach is “full” (unsafe) or “empty” (safe) before anesthesia is using ultrasound to look at the stomach contents. Point-of-care ultrasound (POCUS) is a validated and accurate technique that can be useful but requires additional training and expertise from anesthesiologists.
Leveraging the expertise in POCUS at our institution (UTHealth McGovern Medical School), we conducted a study examining whether patients on a GLP-1 RA had more full stomachs before anesthesia compared to patients not on the drug (control subjects) using gastric ultrasound.
The results were startling: more than half the GLP-1 RA users had a full stomach on gastric ultrasound. This supports observations from multiple case reports of patients on GLP-1 RA having an increased risk of aspirating under anesthesia.
Our study is published in JAMA Surgery:
Sen S, Potnuru PP, Hernandez N, et al. Glucagon-Like Peptide-1 Receptor Agonist Use and Residual Gastric Content Before Anesthesia. JAMA Surg. Published online March 06, 2024. doi:10.1001/jamasurg.2024.0111
